Obesity is a chronic condition defined by an excess amount of body fat. A certain amount of body fat is necessary for storing energy, heat insulation, shock absorption, and other functions.
The foods we eat every day contribute to our well-being. Foods provide us with the nutrients we need for healthy bodies and the calories we need for energy. If we take in more calories than we burn, the extra food turns to fat and is stored in our bodies. If we overeat regularly, we gain weight, and if we continue to gain weight, we may become obese.
All you need to know about – Body mass index (BMI)
Body mass index best defines obesity. A person’s height and weight determines his or her body mass index. The body mass index (BMI) equals a person’s weight in kilograms (kg) divided by their height in meters (m) squared (more information will be found later in the article).
Body Mass Index Chart
| BMI |
Weight Status |
| Below 18.5 |
Underweight |
| 18.5 – 24.9 |
Normal |
| 25.0 – 29.9 |
Overweight |
| 30 or greater |
Obese |
Being a little overweight may not cause many noticeable problems. However, once you are obese, you may develop symptoms that affect your daily life.
Obesity is a chronic medical disease that can lead to diabetes, high blood pressure, obesity associated cardiovascular disease such as heart disease, gallstones, and other chronic illnesses.
Most common causes of obesity
The balance between calorie intake and energy expenditure determines a person’s weight. If a person eats more calories than he or she burns (metabolizes), the person gains weight (the body will store the excess energy as fat). If a person eats fewer calories than he or she metabolizes, he or she will lose weight. Therefore, the most common causes of obesity are overeating and physical inactivity. Ultimately, body weight is the result of genetics, metabolism, environment, behavior, and culture.
- Physical inactivity
- Overeating.
- Genetics.
- A diet high in simple carbohydrates
Risk factors
Obesity usually results from a combination of causes and contributing factors:
Family History
The genes you inherit from your parents may affect the amount of body fat you store, and where that fat is distributed. Genetics may also play a role in how efficiently your body converts food into energy, how your body regulates your appetite and how your body burns calories during exercise.
Obesity tends to run in families. That’s not just because of the genes they share. Family members also tend to share similar eating and activity habits.
Lifestyle choices
Unhealthy diet. A diet that’s high in calories, lacking in fruits and vegetables, full of fast food, and laden with high-calorie beverages and oversized portions contributes to weight gain.
Liquid calories. People can drink many calories without feeling full, especially calories from alcohol. Other high-calorie beverages, such as sugared soft drinks, can contribute to significant weight gain.
Inactivity. If you have a sedentary lifestyle, you can easily take in more calories every day than you burn through exercise and routine daily activities. Looking at computer, tablet and phone screens is a sedentary activity. The number of hours you spend in front of a screen is highly associated with weight gain.
Certain diseases and medications
In some people, obesity can be traced to a medical cause, such as Prader-Willi syndrome, Cushing syndrome and other conditions. Medical problems, such as arthritis, also can lead to decreased activity, which may result in weight gain.
Some medications can lead to weight gain if you don’t compensate through diet or activity. These medications include some antidepressants, anti-seizure medications, diabetes medications, antipsychotic medications, steroids and beta blockers.
Social and economic issues
Social and economic factors are linked to obesity. Avoiding obesity is difficult if you don’t have safe areas to walk or exercise. Similarly, you may not have been taught healthy ways of cooking, or you may not have access to healthier foods. In addition, the people you spend time with may influence your weight — you’re more likely to develop obesity if you have friends or relatives with obesity.
Age
Obesity can occur at any age, even in young children. But as you age, hormonal changes and a less active lifestyle increase your risk of obesity. In addition, the amount of muscle in your body tends to decrease with age. Generally, lower muscle mass leads to a decrease in metabolism. These changes also reduce calorie needs, and can make it harder to keep off excess weight. If you don’t consciously control what you eat and become more physically active as you age, you’ll likely gain weight.
Other factors
Pregnancy. Weight gain is common during pregnancy. Some women find this weight difficult to lose after the baby is born. This weight gain may contribute to the development of obesity in women. Breast-feeding may be the best option to lose the weight gained during pregnancy.
Quitting smoking. Quitting smoking is often associated with weight gain. And for some, it can lead to enough weight gain to qualify as obesity. Often, this happens as people use food to cope with smoking withdrawal. In the long run, however, quitting smoking is still a greater benefit to your health than is continuing to smoke. Your doctor can help you prevent weight gain after quitting smoking.
Lack of sleep. Not getting enough sleep or getting too much sleep can cause changes in hormones that increase your appetite. You may also crave foods high in calories and carbohydrates, which can contribute to weight gain.
Stress. Many external factors that affect your mood and well-being may contribute to obesity. People often seek more high-calorie food when experiencing stressful situations.
Microbiome. Your gut bacteria are affected by what you eat and may contribute to weight gain or difficulty losing weight.
Previous attempts to lose weight. Previous attempts of weight loss followed by rapid weight regain may contribute to further weight gain. This phenomenon, sometimes called yo-yo dieting, can slow your metabolism.
Even if you have one or more of these risk factors, it doesn’t mean that you’re destined to develop obesity. You can counteract most risk factors through diet, physical activity and exercise, and behavior changes.
Symptoms
Although gaining a few extra pounds may seem insignificant as far as a person’s overall health is concerned, weight gain can quickly escalate to a serious medical condition. Symptoms for Adults
Symptoms of obesity can negatively impact one’s daily life.
For adults, symptoms include:
- Excess body fat accumulation (particularly around the waist)
- Shortness of breath
- Sweating (more than usual)
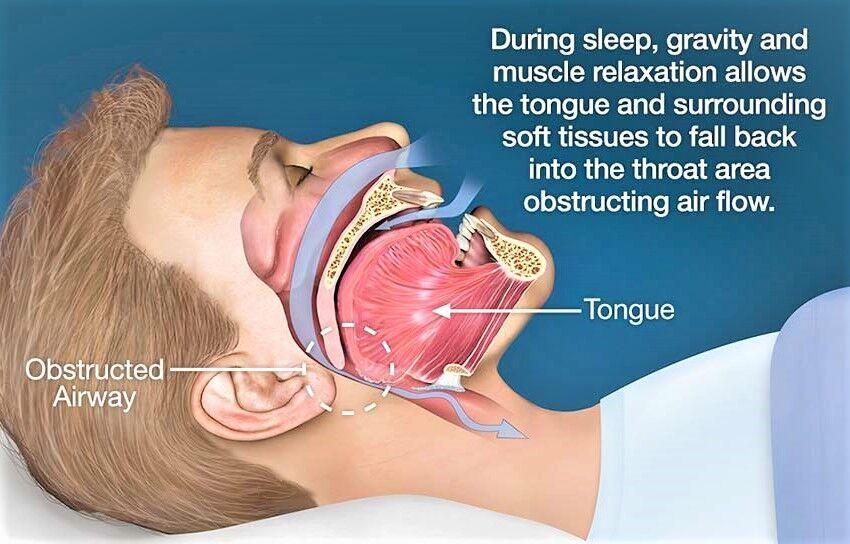
- Snoring
- Trouble sleeping
- Skin problems (from moisture accumulating in the folds of skin)
- Inability to perform simple physical tasks (that one could easily perform before weight gain)
- Fatigue (from mild to extreme)2
- Pain (commonly in the back and joints)
- Psychological impact (negative self-esteem, depression, shame, social isolation)
Common symptoms of childhood obesity may include:
- Eating disorders
- Fatty tissue deposits (may be noticeable in the breast area)
- The appearance of stretch marks on the hips and back
- Acanthosis nigricans (dark velvety skin around the neck and other areas)
- Shortness of breath with physical activity4
- Sleep apnea4
- Constipation
- GI reflux
- Poor self-esteem4
- Early puberty in girls/delayed puberty in boys
- Orthopedic problems (such as flat feet or dislocated hips)

Diagnosis
Diagnosing obesity involves much more than simply stepping onto a scale. In fact, a thorough evaluation of a person’s weight status is a complex procedure that involves taking into consideration many different factors and the use of various tools and diagnostic tests, including body mass index (BMI), waist circumference measurement, physical exams, and lab tests to check for comorbidities.
Self-Checks/At-Home Testing
The most commonly used scale that healthcare providers use to diagnose obesity, is called the body mass index or BMI.
Labs and Tests
It’s important to understand the significance of seeking professional help when it comes to diagnosing childhood, adolescent or adult obesity.
Diagnostic testing for obesity and overweight conditions may involve some lab tests to evaluate the extent of how severely the condition has impacted a person’s overall health and to check for signs of an underlying disease. The lab tests that the healthcare provider will order depend on many factors, such as an individual’s risk factors to obesity-related diseases and current symptoms
Lab tests may include:
Cholesterol levels: Low good cholesterol (HDL) and high bad cholesterol (LDL) levels are commonly associated with obesity
Fasting blood sugar to check for signs of early diabetes
A thyroid test to observe for signs of thyroid disease, commonly linked with obesity
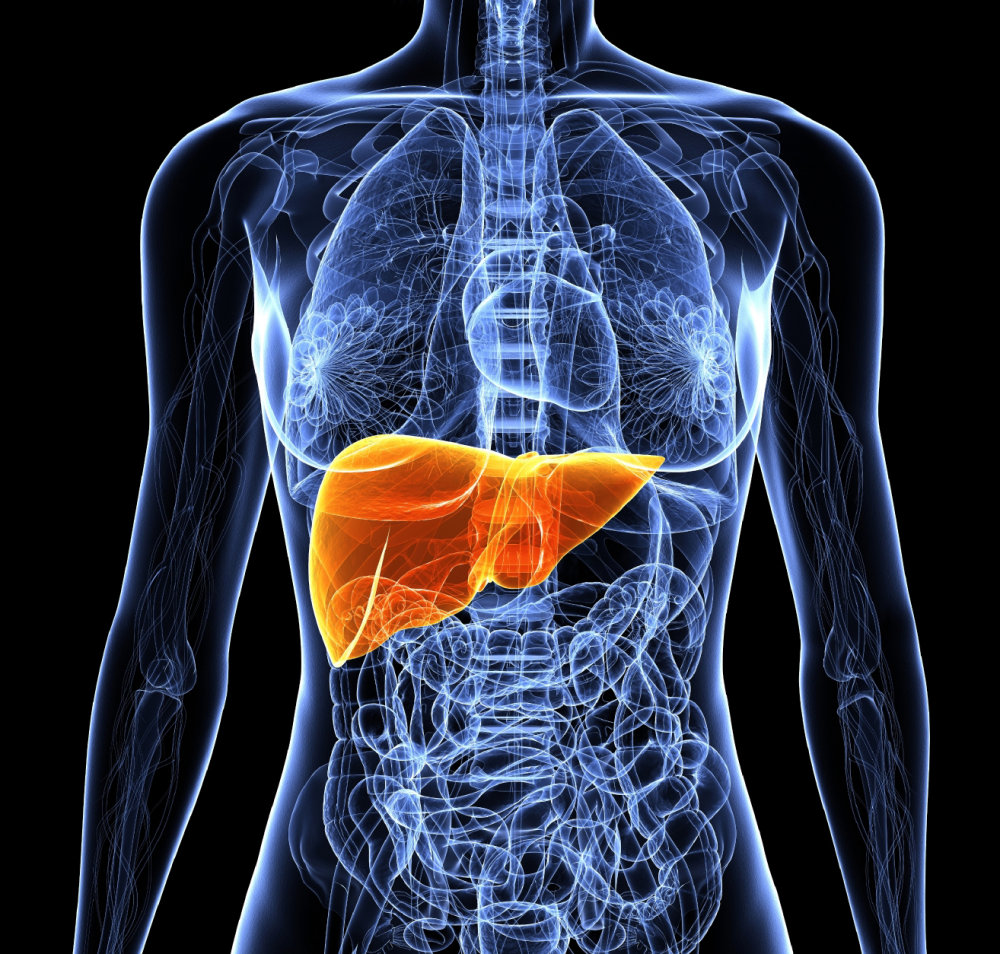
Liver function tests to screen for the potential of fatty liver disease, which often accompanies obesity
Other tests may be ordered by the physician or other healthcare provider to evaluate the overall impact that obesity has on the body. One such test is an electrocardiogram, used to look for signs of heart disease.
Diagnosing Childhood Obesity
To diagnose childhood obesity, the healthcare provider will use a growth chart to evaluate how a child’s weight and height compare to other kids of the same age and sex. For example, a child who is considered in the 90th percentile means that compared with other kids the same age and sex, 90% have a lower weight and BMI.
Because the growth pattern and body frame can differ drastically from one child to the next, pediatricians take several factors into consideration when diagnosing a child’s weight status, these include:
- Growth charts
- Family history of obesity
- Eating habits
- Activity level
- Psychosocial history (includes sleep pattern, mood disorders such as depression, social interactions, and factors such as being bullied)
Other health conditions
Lab tests that may be ordered when a child is suspected of being overweight include:
A cholesterol test
A blood sugar test
Blood tests to check for hormone imbalances
Blood tests to check for obesity-linked conditions
Treatment
The goal of obesity treatment is to reach and stay at a healthy weight. This improves your overall health and lowers your risk of developing complications related to obesity. You may need to work with a team of health professionals — including a dietitian, behavioral counselor or an obesity specialist — to help you understand and make changes in your eating and activity habits.
The initial treatment goal is usually a modest weight loss — 5% to 10% of your total weight. That means that if you weigh 200 pounds (91 kg) and have obesity by BMI standards, you would need to lose only about 10 to 20 pounds (4.5 to 9 kg) for your health to begin to improve. However, the more weight you lose, the greater the benefits.
All weight-loss programs require changes in your eating habits and increased physical activity. The treatment methods that are right for you depend on your obesity severity, your overall health and your willingness to participate in your weight-loss plan.
Dietary changes
Reducing calories and practicing healthier eating habits are vital to overcoming obesity. Although you may lose weight quickly at first, steady weight loss over the long term is considered the safest way to lose weight and the best way to keep it off permanently.
There is no best weight-loss diet. Choose one that includes healthy foods that you feel will work for you. Dietary changes to treat obesity include:
Cutting calories The key to weight loss is reducing how many calories you take in. The first step is to review your typical eating and drinking habits to see how many calories you normally consume and where you can cut back.
Feeling full on less. Some foods — such as desserts, candies, fats and processed foods — contain a large amount of calories for a small portion. In contrast, fruits and vegetables provide a larger portion size with fewer calories.
Making healthier choices. To make your overall diet healthier, eat more plant-based foods, such as fruits, vegetables and whole-grain carbohydrates. Also emphasize lean sources of protein — such as beans, lentils and soy — and lean meats. If you like fish, try to include fish twice a week. Limit salt and added sugar. Eat small amounts of fats, and make sure they come from heart-healthy sources, such as olive, canola and nut oils.
Restricting certain foods. Certain diets limit the amount of a particular food group, such as high-carbohydrate or full-fat foods. Ask your doctor which diet plans have been found effective and which might be helpful for you.
Meal replacements. These plans suggest that you replace one or two meals with their products — such as low-calorie shakes or meal bars — and eat healthy snacks and a healthy, balanced third meal that’s low in fat and calories.
Exercise and activity
Increased physical activity or exercise is an essential part of obesity treatment. Most people who are able to maintain their weight loss for more than a year get regular exercise, even simply Behavior changes
A behavior modification program can help you make lifestyle changes and lose weight and keep it off. Steps to take include examining your current habits to find out what factors, stresses or situations may have contributed to your obesitywalking.
Weight-loss medication
Losing weight requires a healthy diet and regular exercise. But in certain situations, prescription weight-loss medication may help.
Keep in mind, though, that weight-loss medication is meant to be used along with diet, exercise and behavior changes, not instead of them. The main purpose of weight-loss medications, also known as anti-obesity medications, is to help you to stick to a low-calorie diet by stopping the hunger and lack of fullness signals that appear when trying to lose weight.
Your doctor may recommend weight-loss medication if other diet and exercise programs haven’t worked and you meet one of these criteria:
Your body mass index (BMI) is 30 or greater
Your BMI is greater than 27, and you also have medical complications of obesity, such as diabetes, high blood pressure or sleep apnea
Before selecting a medication for you, your doctor will consider your health history, as well as possible side effects. Some weight-loss medications can’t be used by women who are pregnant or by people who take certain medications or have chronic health conditions.
Endoscopic procedures for weight loss
These types of procedures don’t require any incisions in your skin. After you receive anesthesia, flexible tubes and tools are inserted through your mouth and down your throat into your stomach.
There are several different types of endoscopic procedures used for weight loss. One procedure involves placing stitches in your stomach to reduce its size and the amount of food you can comfortably consume. In another endoscopic procedure, doctors insert a small balloon into your stomach. The balloon is filled with water to reduce the amount of space available in your stomach. This helps you feel fuller faster.
These procedures are usually approved for people with BMIs of 30 or above when diet and exercise alone have not been successful. The expected weight loss varies among procedures from 5% to 20% of total body weight loss.
In some people, weight-loss surgery, also called bariatric surgery, is an option. Weight-loss surgery limits the amount of food you’re able to comfortably eat or decreases the absorption of food and calories, or it does both. While weight-loss surgery offers the best chance of losing the most weight, it can pose serious risks.
Weight-loss surgery for obesity may be considered if you have tried other methods to lose weight that haven’t worked and:
You have extreme obesity (BMI of 40 or higher)
Your BMI is 35 to 39.9, and you also have a serious weight-related health problem, such as diabetes or high blood pressure
You’re committed to making the lifestyle changes that are necessary for surgery to work
Weight-loss surgery helps some people lose as much as 35% or more of their excess body weight. But weight-loss surgery isn’t a miracle obesity cure.
It doesn’t guarantee that you’ll lose all of your excess weight or that you’ll keep it off long term. Weight-loss success after surgery depends on your commitment to making lifelong changes in your eating and exercise habits.
Common weight-loss surgeries include:
Gastric bypass surgery. In gastric bypass (Roux-en-Y gastric bypass), the surgeon creates a small pouch at the top of your stomach. The small intestine is then cut a short distance below the main stomach and connected to the new pouch. Food and liquid flow directly from the pouch into this part of the intestine, bypassing most of your stomach.
Adjustable gastric banding. In this procedure, your stomach is separated into two pouches with an inflatable band. Pulling the band tight, like a belt, the surgeon creates a tiny channel between the two pouches. The band keeps the opening from expanding and is generally designed to stay in place permanently.
Biliopancreatic diversion with duodenal switch. This procedure begins with the surgeon removing a large part of the stomach. The surgeon leaves the valve that releases food to the small intestine and the first part of the small intestine (duodenum). Then the surgeon closes off the middle section of the intestine and attaches the last part directly to the duodenum. The separated section of the intestine is reattached to the end of the intestine to allow bile and digestive juices to flow into this part of the intestine.
Gastric sleeve. In this procedure, part of the stomach is removed, creating a smaller reservoir for food. It’s a less complicated surgery than gastric bypass or biliopancreatic diversion with duodenal switch.
Preventing weight regain after obesity treatment
Unfortunately, it’s common to regain weight no matter what obesity treatment methods you try. If you take weight-loss medications, you’ll probably regain weight when you stop taking them. You might even regain weight after weight-loss surgery if you continue to overeat or overindulge in high-calorie foods or high-calorie beverages.
One of the best ways to prevent regaining the weight you’ve lost is to get regular physical activity. Aim for 45 to 60 minutes a day.
Keep track of your physical activity if it helps you stay motivated and on course. As you lose weight and gain better health, talk to your doctor about what additional activities you might be able to do and, if appropriate, how to give your activity and exercise a boost.
Complications
People with obesity are more likely to develop a number of potentially serious health problems:

Heart disease and strokes. Obesity makes you more likely to have high blood pressure and abnormal cholesterol levels, which are risk factors for heart disease and strokes.
Type 2 diabetes. Obesity can affect the way your body uses insulin to control blood sugar levels. This raises your risk of insulin resistance and diabetes.
Certain cancers. Obesity may increase your risk of cancer of the uterus, cervix, endometrium, ovary, breast, colon, rectum, esophagus, liver, gallbladder, pancreas, kidney and prostate.
Digestive problems. Obesity increases the likelihood that you’ll develop heartburn, gallbladder disease and liver problems.
Gynecological and sexual problems. Obesity may cause infertility and irregular periods in women. Obesity also can cause erectile dysfunction in men.
Sleep apnea. People with obesity are more likely to have sleep apnea, a potentially serious disorder in which breathing repeatedly stops and starts during sleep.
Osteoarthritis. Obesity increases the stress placed on weight-bearing joints, in addition to promoting inflammation within the body. These factors may lead to complications such as osteoarthritis.
Quality of life
Obesity can diminish your overall quality of life. You may not be able to do things you used to do, such as participating in enjoyable activities. You may avoid public places. People with obesity may even encounter discrimination.
Other weight-related issues that may affect your quality of life include:
- Depression
- Disability
- Sexual problems
- Shame and guilt
- Social isolation
- Lower work achievement
Prevention
Whether you’re at risk of obesity, currently overweight or at a healthy weight, you can take steps to prevent unhealthy weight gain and related health problems. Not surprisingly, the steps to prevent weight gain are the same as the steps to lose weight: daily exercise, a healthy diet, and a long-term commitment to watch what you eat and drink.
Exercise regularly. You need to get 150 to 300 minutes of moderate-intensity activity a week to prevent weight gain. Moderately intense physical activities include fast walking and swimming.
Follow a healthy-eating plan. Focus on low-calorie, nutrient-dense foods, such as fruits, vegetables and whole grains. Avoid saturated fat and limit sweets and alcohol. Eat three regular meals a day with limited snacking. You can still enjoy small amounts of high-fat, high-calorie foods as an infrequent treat. Just be sure to choose foods that promote a healthy weight and good health most of the time.
Know and avoid the food traps that cause you to eat. Identify situations that trigger out-of-control eating. Try keeping a journal and write down what you eat, how much you eat, when you eat, how you’re feeling and how hungry you are. After a while, you should see patterns emerge. You can plan ahead and develop strategies for handling these types of situations and stay in control of your eating behaviors.
Monitor your weight regularly. People who weigh themselves at least once a week are more successful in keeping off excess pounds. Monitoring your weight can tell you whether your efforts are working and can help you detect small weight gains before they become big problems.
Be consistent. Sticking to your healthy-weight plan during the week, on the weekends, and amidst vacation and holidays as much as possible increases your chances of long-term success.
We’re sure, you now have a fair idea of what Obesity is all about and the way it could impact your life. Please feel free to contact us query@gtsmeditour.com if you’d like to take a second opinion on your condition or undergo treatment for Obesity.













:max_bytes(150000):strip_icc()/GettyImages-523913021-59563bd55f9b5815d93c266d.jpg)