Why is folic acid important?
Vitamin B9 includes both folate and folic acid and is important for several functions in the body.
Folic acid is vital for making red blood cells, as well as:
- the synthesis and repair of DNA and RNA
- aiding rapid cell division and growth
- enhancing brain health, although the evidence is mixed and more research is needed
- age-related hearing loss
It is particularly important for women who are pregnant to consume enough folic acid. This helps prevent the fetus from developing major congenital deformities of the brain or spine, including neural tube defects, such as spina bifida and anencephaly.
Women planning to get pregnant should take folic acid supplements for a full year before conception to reduce the risk of these developments.
Folic acid is thought to play a preventive role in a range of conditions.

Types of diseases which causes by deficiency of Folic acid as follows:
Autism
A recent study connected folic acid deficiency with autism. The investigators concluded: “Periconceptional folic acid [before conception and during early pregnancy] may reduce [autism spectrum disorder] risk in those with inefficient folate metabolism.”
Cleft lip and palate
A literature review carried out in 2014 concluded that folic acid supplementation might reduce the risk of a cleft palate.
Rheumatoid arthritis
Folic acid is often used to support a methotrexate prescription for rheumatoid arthritis.
Methotrexate is an effective medicine for this condition. However, it is also known to remove folate from the body. This can cause gastrointestinal symptoms for between 20 and 65 percent of people who use the drug.
However, folic acid supplements have been shown to reduce the gastrointestinal side effects of methotrexate by 79 percent. Speak to a doctor for recommendations on how much to take, and how often. 1 milligram (mg) per day is often prescribed.
Deficiency
Folic acid deficiency occurs when not enough folate or folic acid is present in the body.
Aside from anemia and congenital deformities, folic acid deficiency can result in other health problems, including:
- a higher risk of developing clinical depression
- possible problems with memory and brain function
- a higher risk of potentially developing allergic diseases
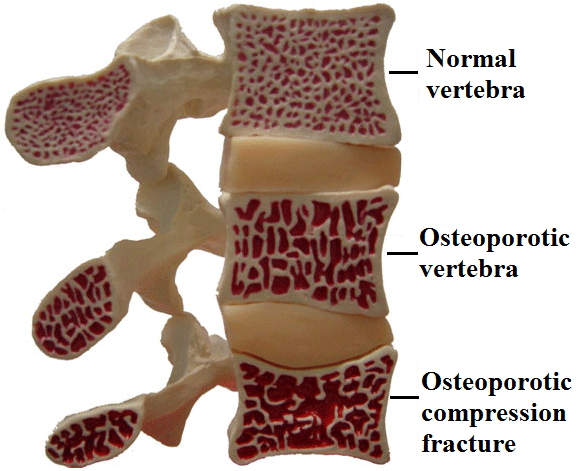
- a higher potential long-term risk of lower bone density
The Medical Journal of Australia advised in January 2011 that the prevalence of folate deficiency in the country had dropped considerably since introducing the compulsory fortification of wheat flour in breadmaking.
Deficiency anemia
Individuals can develop folic acid deficiency anemia if they do not consume enough folic acid.
As folate is important for producing and maintaining red blood cells, inadequate levels can mean that there are not enough red blood cells to supply the body with a healthy level of oxygen.
This condition can appear in people who require higher quantities of folate and are not taking supplements, such as women who are pregnant and lactating.
Folic acid deficiency anemia can occur in people with underlying conditions, such as sickle cell anemia. It can also affect people with conditions that affect folate absorption. Alcohol abuse or kidney disease can reduce the ability of the body to effectively absorb folate.
Some medications, such as those used for treating rheumatoid arthritis, cancer, and seizures, may increase the risk of folic acid deficiency anemia.
The signs and symptoms of folic acid deficiency disease include:
- fatigue
- feeling weak
- sores around the mouth
- memory and cognition difficulties
- irritable mood
- loss of appetite
- weight loss
People with folic acid deficiency anemia are given folic acid pills for daily use. Once folate levels return to normal, the body can produce enough blood cells to allow normal function.
Side effects
There are no serious side effects when taking folic acid. In rare cases, individuals report an upset stomach.
Even if a person takes more folate than needed, there is no cause for concern. Because folic acid is water-soluble, any excess will be naturally passed in urine.
Who should take it?
All women who are pregnant or planning to become pregnant should consume more folic acid, according to March of Dimes, a research organization focused on preventing deformity and death in newborn infants.
They also recommend that women take folic acid before getting pregnant as well as during the first 4 weeks following conception.
Every woman capable of getting pregnant should be taking daily folic acid supplements. Women over the age of 14 years should take 400 micrograms (mcg) per day, and this should increase to 600 mcg during a pregnancy.
Women should maintain a daily intake of 500 mcg.

 Cerebrovascular accident (CVA) – the fancy name for a “stroke”. A blood vessel in the brain may burst causing internal bleeding. Or, a clot may arise in a brain blood vessel (a thrombus), or arise elsewhere (embolus) and travel to get stuck in a brain vessel which then deprives brain tissue of oxygen. Depending upon the area of the brain involved, the patient may suffer paralysis, loss of speech or loss of vision.
Cerebrovascular accident (CVA) – the fancy name for a “stroke”. A blood vessel in the brain may burst causing internal bleeding. Or, a clot may arise in a brain blood vessel (a thrombus), or arise elsewhere (embolus) and travel to get stuck in a brain vessel which then deprives brain tissue of oxygen. Depending upon the area of the brain involved, the patient may suffer paralysis, loss of speech or loss of vision.