Overview
Paralysis, paresis, and plegia are all terms related to loss of motor function, A nervous system problem causes paralysis Even though both paralysis and paresis are related to muscle weakness, there is a significant difference in their severity and how they affect the human body. Plegia, or paralysis, is a complete paralysis of skeletal muscles. whereas paresis is partial or restricted weakness of the muscles. Understanding the differences between paralysis and paresis is essential for proper diagnosis and treatment. Homoeopathic remedies can help improve muscle strength, reduce pain, and support the body’s natural healing processes in addition to this lifestyle changes and physical therapy can also help treat paresis and paralysis.
Paralysis
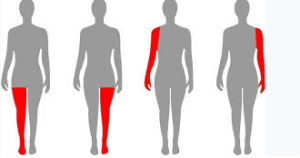
The term paralysis refers to a physical condition that causes a complete loss of muscle function in one or more areas of the body. It occurs when the brain or spinal cord is damaged, resulting in the inability of the affected muscles to move voluntarily. Paralysis can affect different parts of the body, including the arms, legs, face, and trunk. There are different paralysis types, such as:
- Monoplegia: Paralysis in one limb or body part.
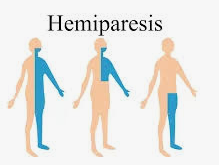
- Hemiplegia: Paralysis on one side of the body.
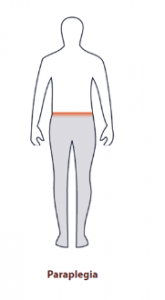
- Paraplegia: Paralysis from the waist down.
- Quadriplegia: Paralysis from the neck down.
Paresis
Paresis, on the other hand, is a medical condition that causes partial loss of muscle function in one or more areas of the body. It occurs when there is damage to the nerves that control muscle movement. Unlike paralysis, paresis only affects the strength and control of the muscles and not their ability to move. There are different types of paresis, such as:
- Hemiparesis: Weakness on one side of the body.
- Paraparesis: Weakness in both legs
- Quadriparesis. Quadriparesis is muscle weakness that affects all four limbs.
- Bell’s palsy. Bell’s palsy is a condition that leads to temporary weakness in your facial muscles, which can cause facial drooping and pain.
- Vocal cord paresis. Vocal cord paresis affects the movement of your vocal cords. The condition often leads to a soft voice or hoarseness, as well as feelings of breathlessness when speaking.
- Gastroparesis. Gastroparesis is a condition where the emptying of the stomach is impaired due to muscle weakness. It’s associated with symptoms like nausea, vomiting, bloating, and feeling full quickly.
- Todd’s paresis. Todd’s paresis is a type of paresis that occurs following a seizure. It’s often associated with paresis in one limb (monoparesis) or on one side of the body (hemiparesis).
- Neurosyphilis. Neurosyphilis occurs when a syphilis infection attacks the nervous system. It can cause paresis as well as headaches, changes in behavior, and dementia.
- Spastic paresis. Spastic paresis is a condition that causes muscle overactivity and spasticity. It’s due to nerve damage that often results from conditions like stroke, MS, and cerebral palsy. This can lead to pain as well as difficulty with activities like walking or getting dressed.
Causes of Paralysis and Paresis
Both paralysis and paresis can have different causes, ranging from traumatic injuries to medical conditions.
Some common causes of paralysis include:
- Traumatic Injuries: Trauma to the brain or spinal cord can cause paralysis. This may occur due to accidents, falls, or sports injuries.
- Strokes: A stroke occurs when the blood supply to the brain is disrupted, causing brain damage. This can lead to paralysis on one side of the body or in specific areas of the body.
- Tumors: Tumors in the brain or spinal cord put pressure on nerves and cause paralysis.
- Neurological Disorders: Certain neurological disorders, such as multiple sclerosis and Parkinson’s disease, can cause paralysis.
- Infections: Some infections can also cause paralysis, such as Lyme disease, polio, and botulism.
Similarly, paresis can also be caused by various factors, such as:
- Nerve Damage: Paresis occurs due to nerve damage caused by trauma or injury, autoimmune disorders, infections, or tumors.
- Medications: Certain medications, such as those used to treat cancer, also cause paresis as a side effect.
- Stroke: Paresis can occur due to a stroke, which is typically less severe than paralysis.
- Spinal Cord Injuries: Injuries to the spinal cord are also one of the main causes of paresis.
- Autoimmune Disorders: Some autoimmune disorders, such as Guillain-Barre syndrome, can cause paresis by attacking the nerves.
Symptoms of Paralysis and Paresis
The symptoms of paralysis and paresis differ depending on the location and extent of the damage to the nerves or muscles. In general, some common symptoms of paralysis include:
- Inability to move the affected body part voluntarily
- Loss of sensation in the affected area
- Muscle stiffness or spasms
- Difficulty breathing, speaking, or swallowing (in severe cases)
On the other hand, symptoms of paresis may include:
- Weakness or reduction in muscle strength in the affected area
- Difficulty performing tasks that require muscle strength or control
- Fatigue or loss of endurance in the affected area
- Muscle twitching or cramping
Treatment of Paresis and Paralysis
Learning to live with paralysis is challenging. It can cause dramatic changes to your life, activities and self-image. These changes can result in mental health issues and depression. Talk with your healthcare provider about getting physical and emotional support. Over time, and with rehabilitation, many people with paralysis learn to adapt. Many people lead independent, active lives with paralysis. People with quadriplegia need lifelong help from others, but their minds can stay active. Homoeopathy is a holistic system of medicine that focuses on treating the individual as a whole rather than just the symptoms. In the case of paresis and paralysis, homoeopathic remedies can help improve muscle strength, reduce pain, and support the body’s natural healing processes.
In addition to homoeopathic remedies, lifestyle changes and physical therapy can also help treat paresis and paralysis. Exercise, massage, and other physical therapy help improve muscle strength and control, reduce pain and stiffness, and promote overall healing and recovery.
In addition if you come across with your lovedones suffering with stroke or spinal injury and looking for medical asssistance you can email us the latest reports at query@gtsmeditour.com or whatsapp us on +91 9880149003 and get the opinion and guidance for the same from the top hospitals Pan India.
Happy To assist..!
Thank you..!