Hepatocellular carcinoma
Hepatocellular carcinoma (HCC) is the most common type of primary liver cancer. Hepatocellular carcinoma occurs most often in people with chronic liver diseases, such as cirrhosis caused by hepatitis B or hepatitis C infection.
Diagnosis
Tests and procedures used to diagnose hepatocellular carcinoma include:
- Blood tests to measure liver function
- Imaging tests, such as CT and MRI with contrast, and advanced imaging procedures, such as magnetic resonance elastography
- Liver biopsy, in some cases, to remove a sample of liver tissue for laboratory testing
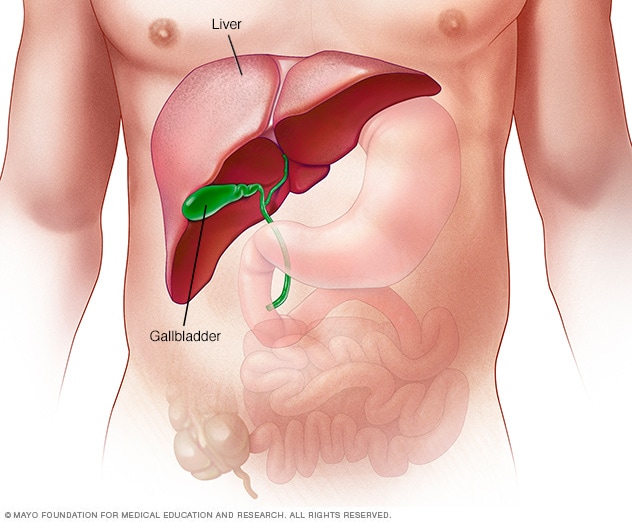
Liver cancer is cancer that begins in the cells of your liver. Your liver is a football-sized organ that sits in the upper right portion of your abdomen, beneath your diaphragm and above your stomach.
Several types of cancer can form in the liver. The most common type of liver cancer is hepatocellular carcinoma, which begins in the main type of liver cell (hepatocyte). Other types of liver cancer, such as intrahepatic cholangiocarcinoma and hepatoblastoma, are much less common.
Not all cancers that affect the liver are considered liver cancer. Cancer that begins in another area of the body — such as the colon, lung or breast — and then spreads to the liver is called metastatic cancer rather than liver cancer. And this type of cancer is named after the organ in which it began — such as metastatic colon cancer to describe cancer that begins in the colon and spreads to the liver. Cancer that spreads to the liver is more common than cancer that begins in the liver cells.
Symptoms
Most people don’t have signs and symptoms in the early stages of primary liver cancer. When signs and symptoms do appear, they may include:
- Losing weight without trying
- Loss of appetite
- Upper abdominal pain
- Nausea and vomiting
- General weakness and fatigue
- Abdominal swelling
- Yellow discoloration of your skin and the whites of your eyes (jaundice)
- White, chalky stools
Causes
It’s not clear what causes most cases of liver cancer. But in some cases, the cause is known. For instance, chronic infection with certain hepatitis viruses can cause liver cancer.
Liver cancer occurs when liver cells develop changes (mutations) in their DNA — the material that provides instructions for every chemical process in your body. DNA mutations cause changes in these instructions. One result is that cells may begin to grow out of control and eventually form a tumor — a mass of cancerous cells.
Risk factors
Factors that increase the risk of primary liver cancer include:
- Chronic infection with HBV or HCV. Chronic infection with the hepatitis B virus (HBV) or hepatitis C virus (HCV) increases your risk of liver cancer.
- Cirrhosis. This progressive and irreversible condition causes scar tissue to form in your liver and increases your chances of developing liver cancer.
- Certain inherited liver diseases. Liver diseases that can increase the risk of liver cancer include hemochromatosis and Wilson’s disease.
- Diabetes. People with this blood sugar disorder have a greater risk of liver cancer than those who don’t have diabetes.
- Nonalcoholic fatty liver disease. An accumulation of fat in the liver increases the risk of liver cancer.
- Exposure to aflatoxins. Aflatoxins are poisons produced by molds that grow on crops that are stored poorly. Crops such as corn and peanuts can become contaminated with aflatoxins, which can end up in foods made of these products. In the United States, safety regulations limit aflatoxin contamination. Aflatoxin contamination is more common in certain parts of Africa and Asia.
- Excessive alcohol consumption. Consuming more than a moderate amount of alcohol daily over many years can lead to irreversible liver damage and increase your risk of liver cancer.
Prevention
Reduce your risk of cirrhosis
Cirrhosis is scarring of the liver, and it increases the risk of liver cancer. You can reduce your risk of cirrhosis if you:
- Drink alcohol in moderation, if at all. If you choose to drink alcohol, limit the amount you drink. For women, this means no more than one drink a day. For men, this means no more than two drinks a day.
- Maintain a healthy weight. If your current weight is healthy, work to maintain it by choosing a healthy diet and exercising most days of the week. If you need to lose weight, reduce the number of calories you eat each day and increase the amount of exercise you do. Aim to lose weight slowly — 1 or 2 pounds (0.5 to 1 kilograms) each week.
- Use caution with chemicals. Follow instructions on chemicals you use at home or at work.
Get vaccinated against hepatitis B
You can reduce your risk of hepatitis B by receiving the hepatitis B vaccine, which provides more than 90 percent protection for both adults and children. The vaccine can be given to almost anyone, including infants, older adults and those with compromised immune systems.
Take measures to prevent hepatitis C
No vaccine for hepatitis C exists, but you can reduce your risk of infection.
- Know the health status of any sexual partner. Don’t engage in unprotected sex unless you’re certain your partner isn’t infected with HBV, HCV or any other sexually transmitted infection. If you don’t know the health status of your partner, use a condom every time you have sexual intercourse.
- Don’t use intravenous (IV) drugs, but if you do, use a clean needle. Reduce your risk of HCV by not injecting illegal drugs. But if that isn’t an option for you, make sure any needle you use is sterile, and don’t share it. Contaminated drug paraphernalia is a common cause of hepatitis C infection. Take advantage of needle-exchange programs in your community and consider seeking help for your drug use.
- Seek safe, clean shops when getting a piercing or tattoo. Needles that may not be properly sterilized can spread the hepatitis C virus. Before getting a piercing or tattoo, check out the shops in your area and ask staff members about their safety practices. If employees at a shop refuse to answer your questions or don’t take your questions seriously, take that as a sign that the facility isn’t right for you.
Ask your doctor about liver cancer screening
For the general population, screening for liver cancer hasn’t been proved to reduce the risk of dying of liver cancer, so it isn’t generally recommended. The American Association for the Study of Liver Diseases recommends liver cancer screening for those thought to have a high risk, including people who have:
- Hepatitis B and one or more of the following apply: are Asian or African, have liver cirrhosis, or have a family history of liver cancer
- Hepatitis C infection and liver cirrhosis
- Liver cirrhosis from other causes, such as an autoimmune disease, excessive alcohol use, nonalcoholic fatty liver disease and inherited hemochromatosis
- Primary biliary cirrhosis
Discuss the pros and cons of screening with your doctor. Together you can decide whether screening is right for you based on your risk. Screening typically involves an ultrasound exam every six months.
Treatment
Which treatment is best for you will depend on the size and location of your hepatocellular carcinoma, how well your liver is functioning, and your overall health.
Hepatocellular carcinoma treatments include:
- Surgery. Surgery to remove the cancer and a margin of healthy tissue that surrounds it may be an option for people with early-stage liver cancers who have normal liver function.
- Liver transplant surgery. Surgery to remove the entire liver and replace it with a liver from a donor may be an option in otherwise healthy people whose liver cancer hasn’t spread beyond the liver.
- Destroying cancer cells with heat or cold. Ablation procedures to kill the cancer cells in the liver using extreme heat or cold may be recommended for people who can’t undergo surgery. These procedures include radiofrequency ablation, cryoablation, and ablation using alcohol or microwaves.
- Delivering chemotherapy or radiation directly to cancer cells. Using a catheter that’s passed through your blood vessels and into your liver, doctors can deliver chemotherapy drugs (chemoembolization) or tiny glass spheres containing radiation (radioembolization) directly to the cancer cells.
- Targeted drug therapy. Targeted drugs, such as sorafenib (Nexavar), may help slow the progression of the disease in people with advanced liver cancer.
- Radiation therapy. Radiation therapy using energy from X-rays or protons may be recommended if surgery isn’t an option. A specialized type of radiation therapy, called stereotactic body radiotherapy (SBRT), involves focusing many beams of radiation simultaneously at one point in your body.
- Clinical trials. Clinical trials give you a chance to try new liver cancer treatments. Ask your doctor whether you’re eligible to participate in a clinical trial.

Post a comment