Overview
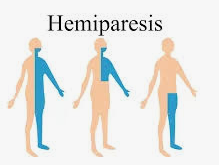
Hemiparesis or hemiplegia are the medical terms, for paralysis of one half of the body. Hemiplegia is a symptom of brain or spinal cord damage where as Hemiparesis refers to weakness in one leg, arm, or side of the face. Hemiplegia describes severe or complete unilateral loss of strength or paralysis. Both may result from a stroke and other conditions. Hemiparesis and hemiplegia may have the same cause, but depending on the severity and location of brain and spinal damage, you may develop one or the other.
Hemiparesis and hemiplegia are both inherently unpredictable, with symptoms that may change over time. Prompt intervention, including extensive physical therapy, can substantially improve the chances of a full recovery. Psychotherapy is also important, since the overwhelming nature of these injuries can interfere with a patient’s ability and willingness to stick with treatment.
Every patient is different, but there is no way to conclusively predict the prognosis of these disorders. Some people spontaneously recover, even with no treatment. Others make little progress, even with extensive treatment. In general, however, the more aggressively a patient works to recover some functionality, the more likely a full or partial recovery becomes.
Hemiparesis and Hemiplegia Causes
There are a number of conditions that can cause hemiparesis or hemiplegia. Examples of hemiparesis and hemiplegia causes include strokes, brain injuries, spinal cord injuries, infections, and a handful of other conditions affecting the central nervous system.
Both hemiparesis and hemiplegia are nervous system disorders, not caused by injury to the affected side of the body. For example, an injury to the spinal cord or brain interferes with the body’s ability to send or receive signals to the region of the body affected by the injury. So, while the left or right side of the body haven’t been damaged directly, the spinal cord injury may cause hemiparesis or hemiplegia.
The most common cause of both injuries is a stroke. Strokes interfere with blood flow to the brain. If a region of the brain that affects movement or perception is affected, hemiparesis or hemiplegia may develop. The affected region is usually the opposite of the side of the brain affected, so an injury to the right side of the brain will affect the left side of the body.
Some other causes of hemiparesis and hemiplegia include:
- Brain infections such as meningitis or encephalitis
- Brain cancer or lesions
- Damage to the neurons due to a degenerative disorder such as Parkinson’s
- Traumatic injuries, such as a blow to the head during a car accident
- Congenital disorders such as cerebral palsy
Rarely, psychological conditions can manifest as hemiparesis or hemiplegia. When this occurs, doctors must treat the psychological issue, not the physical symptoms.
Right Hemiplegia vs Left Hemiplegia
Left hemiplegia is the paralysis of limbs on the left side of the body, while right hemiplegia indicates paralysis on the right side of the body. Like hemiparesis, right or left hemiplegia may be caused by damage to the nervous system.
One common cause of left or right hemiplegia is an incomplete spinal cord injury. In an incomplete SCI, only part of the spinal cord is severed, so there may still be some function below the injury site. For example, an incomplete spinal cord injury in the cervical spinal cord might paralyze the left side of the body while leaving the right side functional — though this isn’t guaranteed because the specific nerves severed may alter the effects of the injury.
Right Hemiparesis vs Left Hemiparesis
As the name implies, right hemiparesis is weakness on the right side of the body, while left hemiparesis is weakness on the left side of the body. What causes this weakness in one side of the body and not the other varies, but damage to the nervous system from injury, infection, or degenerative conditions can result in hemiparesis.
In the case of degenerative conditions such as multiple sclerosis or amyotrophic lateral sclerosis (ALS), hemiparesis may progress into hemiplegia with time.
Did you ever thought why is only one side of the body affected?
Your spinal cord and brain have a left side and a right side. The halves are identical. Each half controls the movements on one side of the body.
An injury to one side of the spinal cord or brain may result in weakness or paralysis on the side of the body that half controls.
If you have multiple strokes on both sides of the brain, you may experience hemiparesis or hemiplegia on both sides of the body.
Symptoms of Hemiplegia & Hemiparesis
Hemiplegia is more severe than hemiparesis. It involves a complete loss of strength or paralysis (inability to move) on one side of the body. It may affect your arm, face, or leg only, or all of them.
Although the paralysis may not be extensive (whole body), it could affect your ability to:
- breath
- swallow
- speak
- control your bladder
- control your bowel
- move one side of your body
It’s common for hemiparesis to unevenly affect one side of the body. The disorder is on a continuum, with symptoms ranging from minor and sporadic to extensive and severe. signs include:
- Difficulties with motor skills, particularly standing.
- Weakness in large areas on one side of the body. For example, a patient might be unable to lift his or her arms.
- Pusher syndrome: a common byproduct of traumatic brain injuries, pusher syndrome causes a person with hemiparesis to shift their weight to the affected side, thereby undermining motor skills and making walking difficult and potentially painful. Doctors use a scale to assess the severity of pusher syndrome. This scale can help doctors make accurate prognostications, in addition to identifying the cause of symptoms.
- Strain on the unaffected side of the body, which may overcompensate for injuries on the hemiparetic side.
- Unusual sensations or tingling on the affected side.
Importantly, doctors will look for injuries on the affected side to rule out other causes, such as pinched nerves, muscle strains, or loss of blood flow.
Diagnosing hemiparesis and hemiplegia
A doctor will most likely use a number of diagnostic procedures and imaging tests to diagnose hemiparesis and hemiplegia.
These might include:
- X-ray
- magnetic resonance imaging (MRI)
- computerized tomography (CT) scan
- electromyography (EMG)
- myelography (imaging test of your spinal cord)
Treatment for Hemiparesis and Hemiplegia
Though hemiparesis and hemiplegia produce different symptoms, they are substantially similar in cause and treatment. To treat either condition, a doctor will first look at what caused the symptoms. When an infection, growth, or other medical issue causes symptoms, a doctor may first address these symptoms. When a stroke is the culprit, the stroke itself cannot be reversed, but a number of treatments may help restore some or all functioning:
- Physical, occupational, or exercise therapy to restore functioning and help the brain work around the injury.
- Assistive devices such as walkers or wheelchairs.
- Occupational therapy to support independence.
- Psychotherapy to address the psychological impact of a severe injury.
- Alternative treatments such as acupuncture and dietary changes.
Conclusion
Though the symptoms are different, the two conditions are essentially different versions of the same underlying problem. Mild to moderate nerve or brain damage will produce hemiparesis, while moderate to severe nerve or brain damage will result in hemiplegia. Moreover, the same injury can produce both symptoms at different times. This is especially true when nerves are compressed or the spinal cord is swollen, since changes in swelling or compression can also produce changes in symptoms.
People living with hemiplegia and hemiparesis usually undergo a combination of rehabilitation therapy, which typically involves physical therapists, mental health professionals, and rehabilitation .
In addition to this if you or your loved ones are looking for medical opinion abroad feel free to email us the medical reports on query@gtsmeditour.com or you can WhatsApp us +91 9880149003
Happy to assist…!
Thank you..!