We can eliminate and protect ourselves against hepatitis B with the help of excellent vaccines available in market. Three injections at regular intervals of time i.e., at 0, 1 and 6 months gives around 90-95% protection against hepatitis. For an effective management apart from vaccination, patients should be checked if they are protected after the vaccination. Hence, it is wise to check one antibody-titer (anti-HBs) after vaccination; a level of more than 10 reflects adequate protection against hepatitis B.
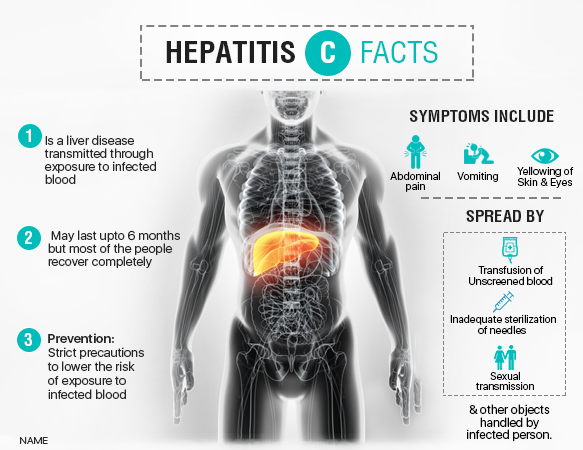
For hepatitis C, unfortunately, there isn’t any vaccine. As both hepatitis B and C are transmitted through blood borne infections, general precautions need to be taken. IV drug abusers are usually prone to hepatitis C. It is important to educate the masses about the dangers of sharing needles or razors with infected individuals.
Another important route of transmission of hepatitis B, and to a lesser extent hepatitis C, is from mother to child. Hence, it is necessary to thoroughly examine expectant mothers during pregnancy. HBV DNA levels should be checked for in the third trimester, and if they are very high (above 108), the expectant mother should undergo treatment. In case the mother is not treated during pregnancy, the newborn baby should be vaccinated within 12 hours of birth, administering both active (vaccine) and passive (immunoglobulin) immunization.
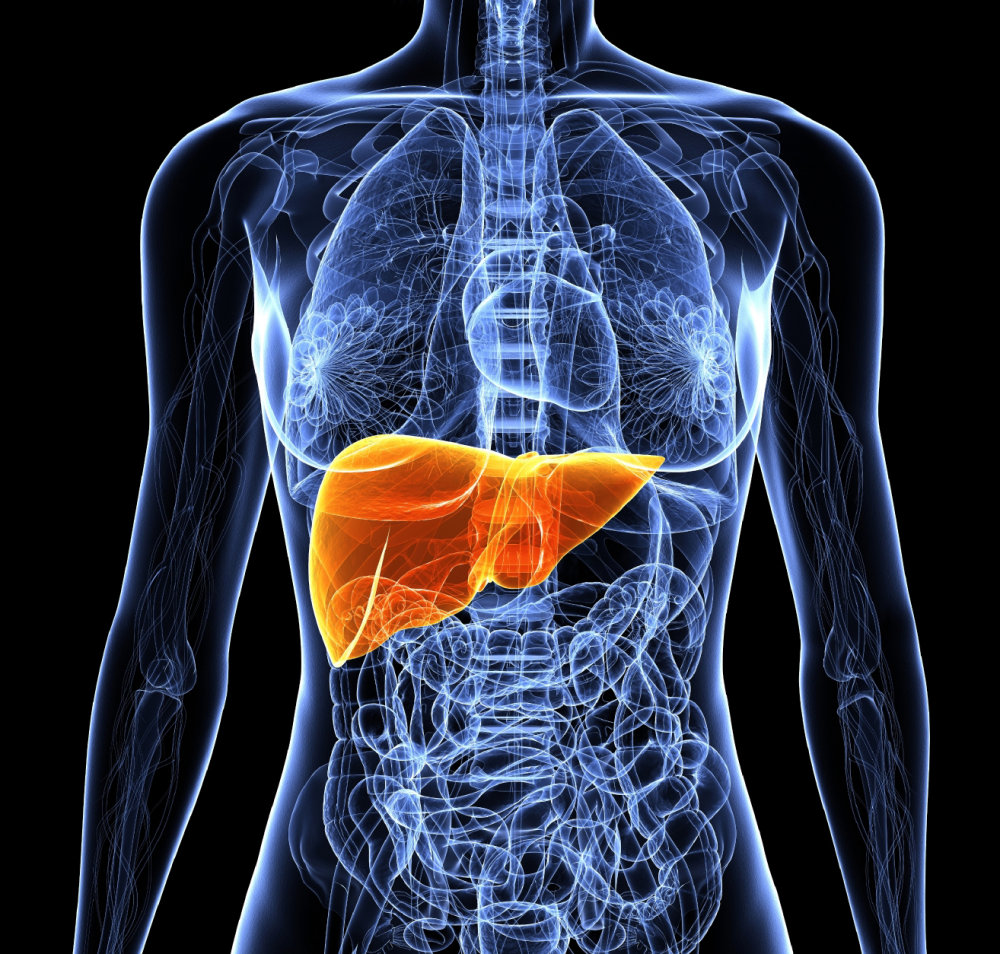
Hepatitis B is a viral infection caused from a small, circular, double stranded DNA virus which predominantly infects the liver in the human body. The most common modes of infection are blood borne or sexual.. Vaginal and seminal secretions contain a large amount of the hepatitis B virus. The most important mode of transmission is the vertical transmission, where the baby gets it from the mother.
Hepatitis B affects the liver, and can either be acute or chronic in nature. Acute infections are self-limiting, i.e., ≥ the disease is healed on its own in 95% of patients due to their strong immune system. Chronic infections have two forms – Chronic active hepatitis and Carrier state hepatitis, which can last for life. In some patients, it can even progress to decompensated liver disease, i.e., cirrhosis, with the end stage being hepatocellular carcinoma. Therefore, it has got a varied presentation, it can be acute/chronic, from where it can advance to form cirrhosis and liver cancer.
Hence, precautionary measures should be adhered to avoid hepatitis B. As a universal health protocol, vaccination of hepatitis B should be administered to every newborn in India. Along with vaccinations, safe sexual practices, avoiding promiscuity and not having multiple sexual partners, avoiding sharing of injections or razors can also help in preventing Hepatitis B infection.
Liver diseases can be categorized into acute infection and chronic infection. Most of the acute infections, in the sub-continents, are hepatitis A and E. Hepatitis A and E are not blood borne infections, but are caused due to fecal-oral route through contaminated water and food. So, safe hygienic practices need to be advocated to avoid this.
For hepatitis B, vaccination is the only precaution.
For hepatitis C, unfortunately, we don’t have any vaccine available.

For alcohol liver diseases causing liver cirrhosis, alcohol is a substance abuse which has the potential to cause permanent liver damage. Avoid drinking alcohol up to a carcinogenic dose. In India, the carcinogenic cut-off level is about 40-80gms/day of alcohol for men and 20-40gms/day for women. In the absence of history of any liver disease, this should not be a potential danger. There are inherited liver diseases where are acquired through genes. One could be hemochromatosis, where the pregnant mother can undergo genetic screening. Lastly, the most common are drug induced liver injuries causing permanent hepatic failure. A proper treatment is needed for control and cure of the disease.