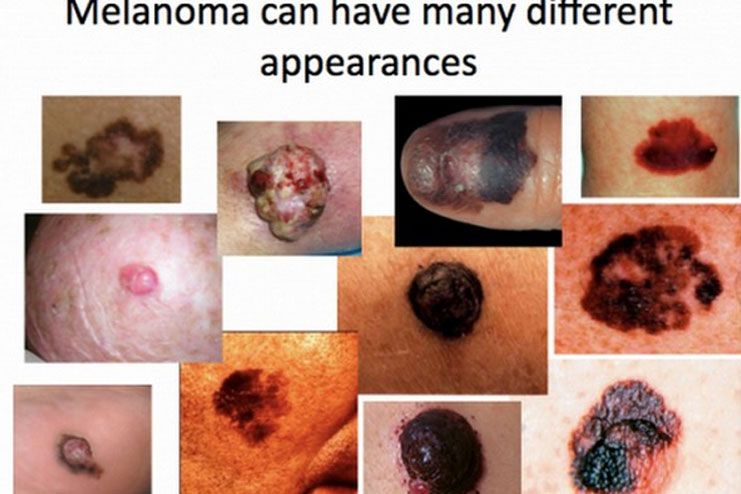
Myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) is a disabling and complex illness.
People with ME/CFS are often not able to do their usual activities. At times, ME/CFS may confine them to bed. People with ME/CFS have overwhelming fatigue that is not improved by rest. ME/CFS may get worse after any activity, whether it’s physical or mental. This symptom is known as post-exertional malaise (PEM). Other symptoms can include problems with sleep, thinking and concentrating, pain, and dizziness. People with ME/CFS may not look ill. However,
- People with ME/CFS are not able to function the same way they did before they became ill.
- ME/CFS changes people’s ability to do daily tasks, like taking a shower or preparing a meal.
- ME/CFS often makes it hard to keep a job, go to school, and take part in family and social life.
- ME/CFS can last for years and sometimes leads to serious disability.
- At least one in four ME/CFS patients is bed- or house-bound for long periods during their illness.
Anyone can get ME/CFS. While most common in people between 40 and 60 years old, the illness affects children, adolescents, and adults of all ages. Among adults, women are affected more often than men. Whites are diagnosed more than other races and ethnicities. But many people with ME/CFS have not been diagnosed, especially among minorities.
Scientists have not yet identified what causes myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS). It is possible that ME/CFS has more than one cause, meaning that patients with ME/CFS could have illness resulting from different causes (see below). In addition, it is possible that two or more triggers might work together to cause the illness.
Some of the areas that are being studied as possible causes of ME/CFS are:
Primary Symptoms:
Also called “core” symptoms, these occur in most patients with ME/CFS. The three primary symptoms required for diagnosis are:
- Greatly lowered ability to do activities that were usual before the illness. This drop in activity level occurs along with fatigue and must last six months or longer. People with ME/CFS have fatigue that is very different from just being tired. The fatigue of ME/CFS:
- Can be severe.
- Is not a result of unusually difficult activity.
- Is not relieved by sleep or rest.
- Was not a problem before becoming ill (not life-long).
- Worsening of ME/CFS symptoms after physical or mental activity that would not have caused a problem before illness. This is known as post-exertional malaise (PEM). People with ME/CFS often describe this experience as a “crash,” “relapse,” or “collapse.” It may take days, weeks, or longer to recover from a crash. Sometimes patients may be house-bound or even completely bed-bound during crashes. People with ME/CFS may not be able to predict what will cause a crash or how long it will last. As examples:
- Attending a child’s school event may leave someone house-bound for a couple of days and not able to do needed tasks, like laundry.
- Shopping at the grocery store may cause a physical crash that requires a nap in the car before driving home or a call for a ride home.
- Taking a shower may leave someone with severe ME/CFS bed-bound and unable to do anything for days.
- Sleep problems. People with ME/CFS may not feel better or less tired, even after a full night of sleep. Some people with ME/CFS may have problems falling asleep or staying asleep.
In addition to these core symptoms, one of the following two symptoms is required for diagnosis:
- Problems with thinking and memory. Most people with ME/CFS have trouble thinking quickly, remembering things, and paying attention to details. Patients often say they have “brain fog” to describe this problem because they feel “stuck in a fog” and not able to think clearly.
- Worsening of symptoms while standing or sitting upright. This is called orthostatic intolerance. People with ME/CFS may be lightheaded, dizzy, weak, or faint while standing or sitting up. They may have vision changes like blurring or seeing spots.
Other Common Symptoms:
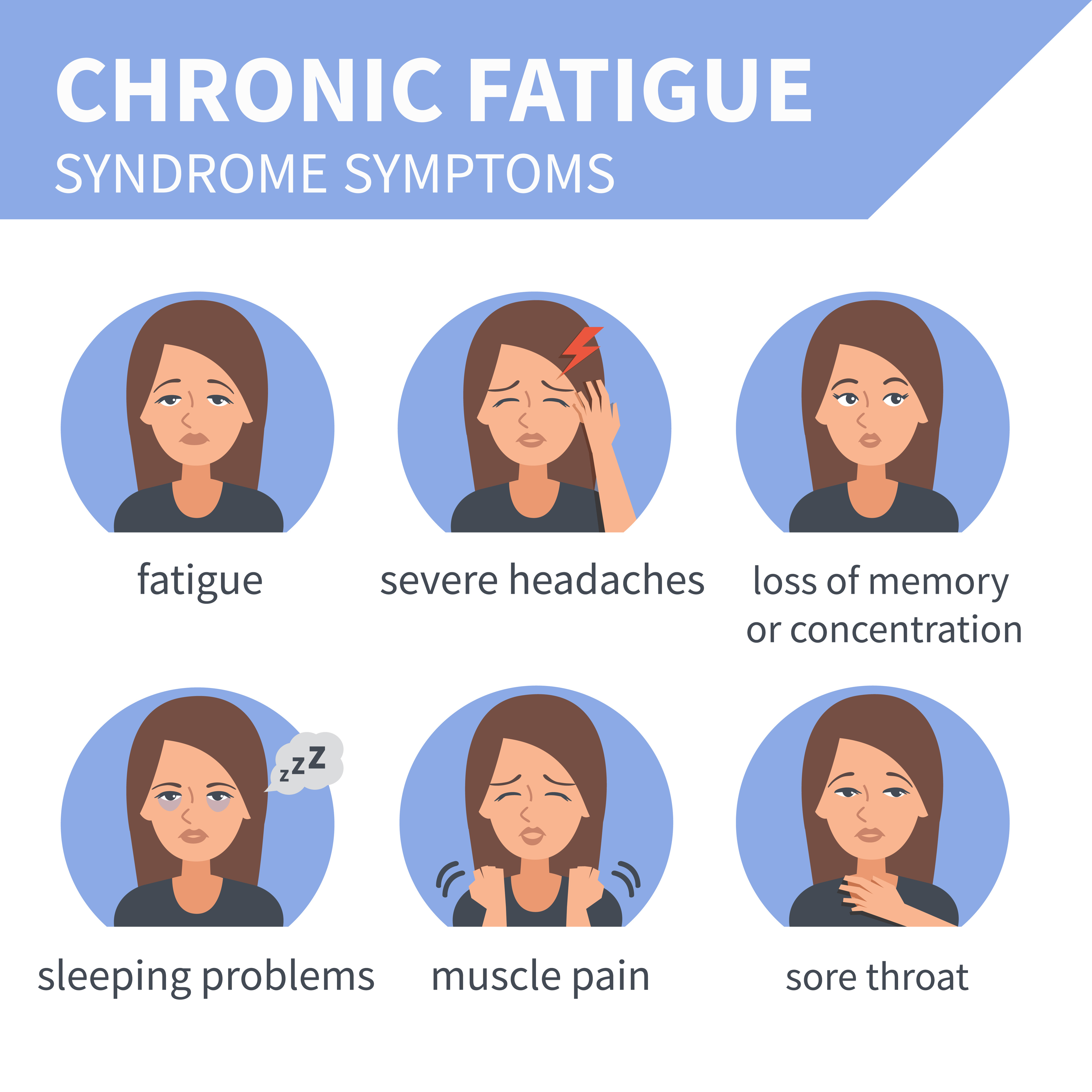
Many but not all people with ME/CFS have other symptoms.
Pain is very common in people with ME/CFS. The type of pain, where it occurs, and how bad it is varies a lot. The pain people with ME/CFS feel is not caused by an injury. The most common types of pain in ME/CFS are:
- Muscle pain and aches
- Joint pain without swelling or redness
- Headaches, either new or worsening
Some people with ME/CFS may also have:
- Tender lymph nodes in the neck or armpits
- A sore throat that happens often
- Digestive issues, like irritable bowel syndrome
- Chills and night sweats
- Allergies and sensitivities to foods, odors, chemicals, or noise
Treatments:
There is no cure or approved treatment for myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS). However, some symptoms can be treated or managed. Treating these symptoms might provide relief for some patients with ME/CFS but not others. Other strategies, like learning new ways to manage activity, can also be helpful.
1.Depression, Stress, and Anxiety
Adjusting to a chronic, debilitating illness sometimes leads to other problems, including depression, stress, and anxiety. Many patients with ME/CFS develop depression during their illness. When present, depression or anxiety should be treated. Although treating depression or anxiety can be helpful, it is not a cure for ME/CFS.
Some people with ME/CFS might benefit from antidepressants and anti-anxiety medications. However, doctors should use caution in prescribing these medications. Some drugs used to treat depression have other effects that might worsen other ME/CFS symptoms and cause side effects. When healthcare providers are concerned about patient’s psychological condition, they may recommend seeing a mental health professional.
Some people with ME/CFS might benefit from trying techniques like deep breathing and muscle relaxation, massage, and movement therapies (such as stretching, yoga, and tai chi). These can reduce stress and anxiety, and promote a sense of well-being.
2.Dizziness and Lightheadedness (Orthostatic Intolerance)
Some people with ME/CFS might also have symptoms of orthostatic intolerance that are triggered when-or made worse by-standing or sitting upright. These symptoms can include:
- Frequent dizziness and lightheadedness
- Changes in vision (blurred vision, seeing white or black spots)
- Weakness
- Feeling like your heart is beating too fast or too hard, fluttering, or skipping a beat
For patients with these symptoms, their doctor will check their heart rate and blood pressure, and may recommend they see a specialist, like a cardiologist or neurologist.
For people with ME/CFS who do not have heart or blood vessel disease, doctor might suggest patients increase daily fluid and salt intake and use support stockings. If symptoms do not improve, prescription medication can be considered.
3. Sleep Problems
Patients with ME/CFS often feel less refreshed and restored after sleep than they did before they became ill. Common sleep complaints include difficulty falling or staying asleep, extreme sleepiness, intense and vivid dreaming, restless legs, and nighttime muscle spasms.
Good sleep habits are important for all people, including those with ME/CFS. Some common tips for good sleep are:
- Start a regular bedtime routine with a long, calming wind-down period.
- Go to bed at same time each night and wake up at same time each morning.
- Limit daytime naps to 30 minutes in total during the day.
- Remove all TVs, computers, phones, and gadgets from bedroom.
- Use the bed only for sleep and sex and not for other activities (avoid reading, watching TV, listening to music, or using phones).
- Control noise, light, and temperature.
- Avoid caffeine, alcohol, and large meals before bedtime.
- Avoid exercise right before going to bed. Light exercise and stretching earlier in the day, at least four hours before bedtime, might improve sleep.
When people try these techniques but are still unable to sleep, their doctor might recommend taking medicine to help with sleep. First, people should try over-the-counter sleep products. If this does not help, doctors can offer a prescription sleep medicine, starting at the smallest dose and using for the shortest possible time.
People might continue to feel unrefreshed even after the medications help them to get a full night of sleep. If so, they should consider seeing a sleep specialist. Most people with sleep disorders, like sleep apnea (brief pause in breathing during sleep) and narcolepsy (uncontrollable sleeping), respond to therapy. However, for people with ME/CFS, not all symptoms may go away.








 .
.